
The near term future is looking much brighter than it was in March 2020, when I published my first set of scenarios exploring how the COVID-19 pandemic might play out. While the death toll in the US has surpassed 600,000 (a grim statistic that falls between the middle and worst case scenarios I explored at the beginning of the COVID-19 shutdowns), cases and deaths are both trending downwards. Over forty percent of the US population is vaccinated, including over 76% of people sixty-five or older (the age cohort most grievously damaged by the coronavirus). Many states and municipalities are lifting restrictions, and as of the end of April, over 70 percent of US museums had reopened to the public.
This progress doesn’t mean that museums can relax their planning, trusting that everything will continue to get better over the remainder of the year. The current promising trajectory could be disrupted by a number of factors, and scenario planning is just as important now as it was in spring 2020. In today’s post, I summarize recent findings that suggest a scenario in which the US recovery from the pandemic slows, and we experience new surges in some areas.
Last week the US Centers for Disease Control and Prevention announced that the Delta variant of the novel coronavirus, also known as B.1.617.2, is now considered a “variant of concern.” Research suggests that this variant, which was first identified in India, is 60 percent more contagious than the Alpha strain that originally dominated the US, and is associated with double the risk of hospitalization. While the Moderna and Pfizer vaccines seem to provide good protection against Delta, there is some laboratory evidence that they may somewhat less effective.
At the time of the CDC announcement, the Delta variant was responsible for 10.3 percent of US Covid-19 cases, up 6 percent from only a week ago. Ten percent is about the “tipping point” at which when Delta began spreading rapidly through the UK, where it is now the dominant strain. Dr. Eric Topol, the founder and director of the Scripps Research Translational Institute, recently noted that as the Delta variant “doubles every seven to 10 days…when it gets to three weeks from now, this variant will be dominant. That means we have two to three weeks to just go flat out with vaccination to stop this trend.”
Unfortunately, it doesn’t look likely we’ll be able to supercharge the vaccination rate in the US. Although 43.9 percent of the US population is fully vaccinated, the rate at which people are getting vaccinated has been slowing down, and some states have stalled at dangerously low levels: Mississippi 29%; Alabama <31%; Arkansas, <33%; Louisiana, Georgia, and Wyoming all <34%, according to CDC data. Elsewhere in the country, there are localized communities with very low vaccination rates. (For example, in Borough Park, NYC less than 11% of the population is vaccinated, due to vaccine hesitancy among Hasidic Jews). And some demographic groups, such as children under the age of 12 and people who are immunocompromised, remain at risk because they aren’t yet eligible for or can’t safely use the vaccine.
For all these reasons, museums—particularly museums in states or communities with low vaccination rates—should be prepared for the possibility of a local surge in COVID-19 cases, hospitalizations, and deaths, and reimposition of precautions such as closures, limits on attendance, and mandatory masking. (The contagiousness and severity of Delta has prompted the British government to delay easing their coronavirus restrictions by a full month.) Even local surges could affect attitudes nationally about continued mask use, distancing, and willingness to visit museums.
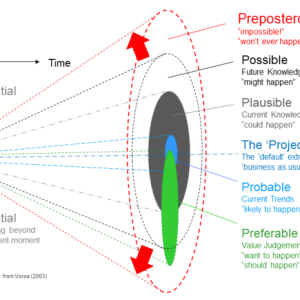
This isn’t a forecast or prediction, it’s just sketching, for your radar, a near term future that falls well within the bounds of the Cone of Plausibility. (I’d peg it to the “plausible” Zone in the following diagram of the Cone—the area which current knowledge suggests a set of conditions “could happen.”)
What can museum people do?
- Monitor local COVID metrics and announcements from the CDC, state and local government to track the effect Delta is having on your community.
- Prepare a plan for responding to a COVID resurgence—including communications, internal procedures, and budgeting for reclosing and reopening.
- Finally, even if things continue to improve in your community, remember that everyone is recovering (physically and psychologically) at their own rate, and for many the trauma of the past year will linger for a long time. Your staff and your community continue to need your support and understanding as we emerge from the pandemic.
Never assume you know what the future will be, especially in such an unsettled year. Spending a little mental and emotional energy on scenarios now will make a potential crisis less costly.
Skip over related stories to continue reading article









Comments